Diabetic Neuropathy and the Risk of Diabetic Foot Ulcers

Apr 21, 2024

Dr Tan Yih Kai
Diabetic neuropathy increases the risk of foot ulcers by reducing sensation, making it hard to detect injuries that can lead to gangrene and serious infections.
Introduction
Diabetic neuropathy is a common and serious complication of diabetes, affecting up to 50% of individuals with diabetes during their lifetime. It encompasses a group of nerve disorders caused by diabetes, which can significantly impair quality of life and increase the risk of further complications, such as diabetic foot ulcers. This article explores the types of diabetic neuropathy—sensory, motor, and autonomic—and the development of diabetic foot ulcers, providing essential insights for management and prevention.
What is Diabetic Neuropathy?
Diabetic neuropathy refers to the damage inflicted on nerves due to high blood sugar levels associated with diabetes. Over time, elevated glucose levels can deteriorate the small blood vessels that supply vital nutrients and oxygen to the nerves, leading to neuropathy. This condition can manifest in various forms, primarily categorized into sensory, motor, and autonomic neuropathy, each affecting different nerve groups and leading to distinct complications.
1. Sensory Neuropathy
Sensory neuropathy affects the nerves responsible for sensation. It is the most common form of neuropathy in people with diabetes. It typically starts in the feet and can spread to the hands. Symptoms include numbness, tingling, pain, or weakness in the affected areas. The loss of sensation means that injuries, cuts, or blisters can go unnoticed, setting the stage for severe infections or ulcers.
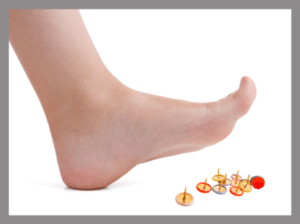
Sensory Neuropathy with Lack of Pain Sensation
2. Motor Neuropathy
Motor neuropathy involves the nerves that control muscle movement. When these nerves are damaged, muscles might not function properly, leading to muscle weakness and imbalances in the foot’s structure. This can affect a person’s balance and coordination, increasing the risk of falls and injuries. Furthermore, muscle weakness can contribute to deformities in the feet, such as claw toes, hammertoes, or the collapse of the foot arch, which alter foot biomechanics and, thus, abnormal gait. These deformities can also change the way weight is distributed across the foot, leading to abnormal pressure points when standing, walking, or running. These abnormal pressure points of the foot are typically the ball of the foot or the underside of the toes to endure excessive stress. Over time, this stress over the pressure areas can lead to callus formation and, eventually, skin breakdown beneath these hardened areas, forming ulcers.
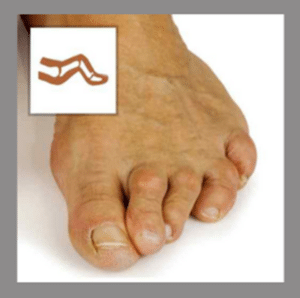
Hammer Toe Deformity
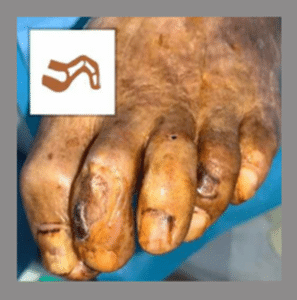
Claw Toe Deformity
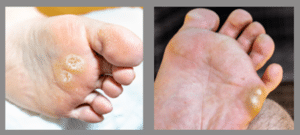
Calluses on Pressure Points
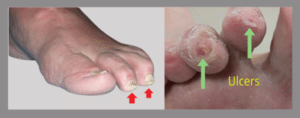
Claw Toes: Pressure Points and Ulcers
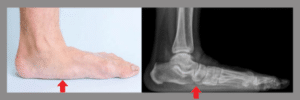
Flat Foot: Pressure Point
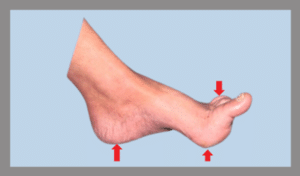
High-arch Foot: Pressure Points
3. Autonomic Neuropathy
Autonomic neuropathy affects the nerves that control involuntary bodily functions, including heart rate, digestion, and bladder control. Relevant to foot health, autonomic neuropathy can impair sweat and oil production in the feet. This results in dry, cracked skin, which is more susceptible to infection and the development of ulcers.

Diabetic Autonomic Neuropathy: Dry Skin
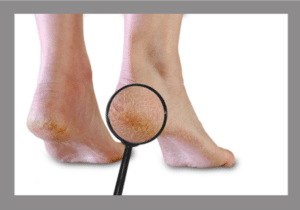
Diabetic Autonomic Neuropathy: Dry and Cracked Skin
Diabetic Foot Ulcers: A Dangerous Complication
Diabetic foot ulcers are open sores or wounds that typically occur on the bottom of the foot. In individuals with diabetes, these ulcers often result from a combination of neuropathy, poor circulation (another complication of diabetes), and an inability to heal properly. Foot deformities and poor footwear can also create constant pressure points and contribute to the formation of ulcers.
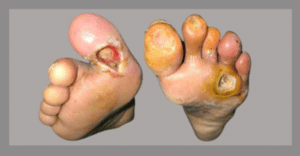
Diabetic Foot Ulcers
Reduced Blood Flow (Peripheral Arterial Disease)
Although not a direct result of neuropathy, many individuals with diabetes also suffer from peripheral arterial disease (PAD), which reduces blood flow to the feet. Reduced blood flow impairs healing and increases the risk of ulcers becoming infected, compounding the problem initiated by neuropathy.
Here are some hard facts concerning diabetic PAD:
• 70% of diabetic wounds/ ulcers involve PAD.
• Almost 85% of amputations related to diabetes are preceded by ulcers, indicating that many of these amputations could be prevented.
• Two-thirds of older adults who undergo amputation fail to regain their independence.
• Approximately 70% of individuals who undergo amputation pass away within five years.
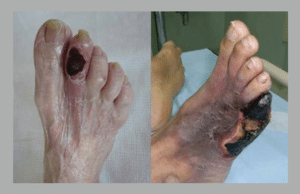
Diabetic Foot Gangrene
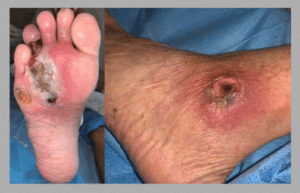
Diabetic Foot Gangrene with Infection
Risk Factors and Prevention
Key risk factors for diabetic foot ulcers include:
1. Duration of Diabetes: Longer duration increases the risk.
2. Poor Blood Glucose Control: High blood sugar levels can lead to nerve damage and poor circulation.
3. Diabetic Neuropathy: Nerve damage that causes loss of sensation in the feet.
4. Peripheral Arterial Disease (PAD): Reduced blood flow to the feet, impairing wound healing.
5. Foot Deformities: Such as hammertoes, bunions, or Charcot joints, which can create pressure points.
6. Inappropriate Footwear: Shoes that do not fit well can cause blisters, sores, and ulcers.
7. Previous Foot Ulcers: History of foot ulcers increases the likelihood of future occurrences.
8. Poor Foot Hygiene and Care: Neglecting foot care can lead to conditions that promote ulcer formation.
9. Smoking: Impairs circulation, exacerbating risks associated with poor blood flow.
10. Obesity: Increases pressure on the feet and complicates diabetes management.
Preventive measures
Preventive measures for diabetic foot ulcers are crucial for maintaining foot health and avoiding complications. Here are key strategies to consider:
1. Regular Foot Inspections: Check your feet daily for cuts, blisters, redness, swelling, or nail problems.
2. Manage Blood Glucose Levels: Maintain your blood sugar within the recommended range to help prevent further nerve damage and improve healing.
3. Wear Appropriate footwear: Choose well-fitting, comfortable shoes that provide good support and cushioning. Avoid tight shoes and pointed toes.
4. Keep Feet Clean and Moisturized: Wash your feet daily and dry them gently, especially between the toes. Apply a moisturizer to prevent dry skin from cracking.
5. Trim Nails Carefully: Cut nails straight across and file the edges. Avoid cutting nails too short to prevent injury.
6. Avoid Walking Barefoot: Always wear shoes or slippers, even indoors, to avoid injuries.
7. Stop Smoking: Smoking impairs circulation and reduces the amount of oxygen that reaches the feet, which can hinder wound healing.
8. Regular Check-ups with Healthcare Provider: Have your feet examined by a healthcare professional at least once a year – more often if you have known risk factors for foot problems.
9. Exercise Regularly: Physical activity can improve circulation and help maintain healthy blood sugar levels.
10. Educate Yourself and Family: Learn about the risks and preventative care for diabetic foot issues. Educate family members so they can help with inspections and recognize early signs of complications.
Implementing these measures can significantly reduce the risk of developing foot ulcers and ensure early detection and treatment of potential problems.
Conclusion
Diabetic neuropathy and the resulting risk of foot ulcers are significant concerns for individuals with diabetes. Understanding the different types of neuropathy and their implications can help in early identification and appropriate management. By integrating comprehensive foot care into the daily routine and maintaining optimal control of blood glucose levels, individuals with diabetes can significantly reduce their risk of developing serious foot complications. Remember, early intervention and consistent management are key to preventing the severe consequences of diabetic neuropathy.







